- 9
- 46
- 26
- 155
- 5
- 37
70 something year old patient with incidental aortic root aneurysm with severe aortic valve insufficiency identified during pre-operative clearance for knee replacement. Underwent biocomposite aortic root replacement with ascending replacement. Distal anastomosis performed under moderate hypothermic circulatory arrest with antegrade cerebral perfusion. You can see aortic valve, coronary arteries, and into LV cavity. Patient also had anomalous chordal structure in LVOT that was removed. Uneventful post-op course and home in 5 days.
- 4
- 7
- 2
- 17
The patient was a middle-aged Caucasian man with chronic pain related to a work injury to the right wrist. A prior surgery did not relieve his pain and he was on multiple pain medications. The patient died suddenly after an unwitnessed cardiopulmonary arrest.
- 4
- 37
- 12
- 47
- 14
- 72
She was killed by being stabbed in throat. Then her assailant had postmortem shoved deep into her anal passage a long katana or something. Also shows her brain autopsy.
- 12
- 67
close-up version of this post
https://watchpeopledie.tv/h/medical/post/11928/archive-mmc-after-an-unknown-flesheating
- 7
- 14
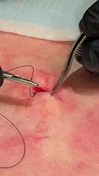
The management of dislocated posterior chamber intraocular lenses (IOLs) involves a systematic approach to address the displacement of the IOL from its intended position within the eye. The dislocation may occur as a result of trauma, zonular weakness, or surgical complications. The following steps outline the management of dislocated posterior chamber IOL:
Clinical Assessment:
Conduct a thorough clinical examination to assess the extent of IOL dislocation.
Evaluate visual acuity, intraocular pressure, and anterior and posterior segment findings.
Determine the cause of dislocation, whether it is traumatic or due to other factors.
Imaging Studies:
Utilize imaging modalities such as ultrasound or optical coherence tomography (OCT) to obtain detailed information about the location and extent of IOL dislocation.
Assess the integrity of the capsular bag and zonular support.
Medical Management:
Manage any associated inflammation or complications, such as uveitis, with appropriate anti-inflammatory medications.
Stabilize intraocular pressure if elevated.
Repositioning:
Attempt to reposition the dislocated IOL to its original location whenever feasible.
Various techniques may be employed, including using specialized instruments or manipulating the IOL through small incisions.
Surgical Intervention:
If repositioning is unsuccessful or not possible, surgical intervention may be required.
Options include re-fixation of the dislocated IOL using sutures or the implantation of a new IOL.
Consideration should be given to the choice of IOL, potential need for additional capsular support, and the overall surgical approach.
Scleral Fixation:
Scleral fixation of the IOL may be performed using sutures to secure the IOL to the sclera.
This technique provides stability and support for the IOL in the absence of intact zonules.
Secondary IOL Implantation:
If the dislocated IOL cannot be salvaged, the implantation of a secondary IOL may be considered.
The type and power of the secondary IOL should be carefully selected based on the patient's refractive needs and anatomical considerations.
Postoperative Monitoring:
Postoperative follow-up is essential to monitor for any complications, assess visual outcomes, and ensure the stability of the repositioned or newly implanted IOL.
Patient Education:
Educate the patient about the surgical procedure, potential risks, and expected outcomes.
Emphasize the importance of regular follow-up visits for ongoing monitoring and management.
Collaboration with Specialists:
In complex cases or cases involving significant ocular comorbidities, collaboration with vitreoretinal or corneal specialists may be necessary.
The management of dislocated posterior chamber IOLs requires a tailored approach based on individual patient characteristics, underlying causes, and the surgeon's expertise.
- 7
- 29
Four persons were killed after a speeding ambulance crashed into a toll plaza after skidding off a wet road in Karnataka’s Udupi district on Wednesday.
The incident happened at Shirur toll gate counter when the vehicle was proceeding to Kundapur hospital from Honnavar.
In a chilling video that has surfaced online, the ambulance driver is seen losing control over the vehicle while making an attempt to cross the toll gate. Within seconds, it rammed into the toll plaza and overturned.
The incident happened at around 4.07 pm when the ambulance, carrying a patient named Gajanan Nayak, along with his wife and relatives, was heading to a Kundapur hospital.
While the occupants got thrown out of the vehicle due to the impact of the crash, the ambulance rammed a staff working at the plaza.
The patient, his wife and their relatives were seriously injured and were rushed to a nearby hospital, where they breathed their last.
The deceased persons have been identified as Manjunatha Madeva Naika, Lokesh Naika, Jyothi Naika and Gajanana Laxman Naika, all residents of Hadigeri Honnavar. The toll plaza staff — identified as Sambaj Ghorpade — sustained serious injuries.
The Byndoor police have registered a case and an investigation is on. Ambulance driver Roshan Rodrigues is out of danger.
- 15
- 12
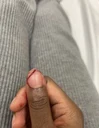
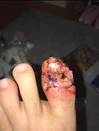
No it's kind of weird because 1. i felt it die and 2. i know what my fingers and toes are gonna look like when i die now💀 Also i'll probably have to just get the shit removed, i can see the layers of my skin. My whole dermis is showing on that part of my finger and i have no clue what that white shit is
- 7
- 44
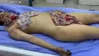
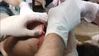
As a former medic I thought it would be interesting to start a small series on different injuries types. If you enjoy the information & photos consider a upvote & follow for my effort post! 
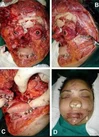
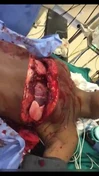
A degloving injury is a type of avulsion in which an extensive section of skin is completely torn off the underlying tissue, severing its blood supply. It is named by analogy to the process of removing a glove.
The causes of degloving can vary, but they often occur when someone's hand or arm gets stuck in a machine or when they are involved in a car crash. Treatment for degloving injuries can vary depending on the severity of the injury, but often includes surgery and skin grafts.
All sorts of events can lead to this type of injury. Car crashes, falls, or getting caught in machinery are all common causes. However, there are also less obvious things that can cause degloving injuries, like contact with chemicals or extreme weather conditions.
Typically, degloving injuries affect the extremities and limbs; in these cases, they are frequently associated with underlying fractures. Any injury which would induce degloving of the head or torso is likely to be lethal. However, controlled facial degloving is often featured in plastic surgery.
Degloving injuries invariably require major surgical interventions. Treatment options include replantation or revascularization of the degloved skins, or when these are not possible, skin grafts or skin flaps. While the preservation of the extremities and limbs is normally preferred, in some cases amputations may be advised or required. Post-operative physiotherapy is of particular importance for degloving injuries involving the hand.
Many small mammals are able to induce degloving of their tails to escape capture; this is comparable to tail autotomy in reptiles.
Sources:















































.webp?x=8)


















 Posting medical gore is my thing
Posting medical gore is my thing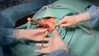





























 Slavshit
Slavshit

 Sandshit
Sandshit
