- 56
- 45
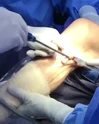
A vasectomy is a form of male birth control that cuts the supply of sperm to your semen. It's done by cutting and sealing the tubes that carry sperm. Vasectomy has a low risk of problems and can usually be performed in an outpatient setting under local anesthesia.
- 3
- 17
A) Intra-operative image of the right hemipelvis fracture fragments trapping a loop of ileum within the right obturator foramen. B) Resected portion of ileum containing perforation secondary to pelvic fracture fragments.
SOURCE: https://www.sciencedirect.com/science/article/pii/S2352644022000310
- 7
- 61
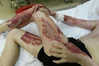
Toxic epidermal necrolysis (TEN) is a rare and serious skin condition. Often, it's caused by an adverse reaction to medication like anticonvulsants or antibiotics.
The main symptom is severe skin peeling and blistering. The peeling progresses quickly, resulting in large raw areas that may ooze or weep. It also affects the mucous membranes, including the mouth, throat, eyes, and genital region.
CAUSES
Because TEN is so rare, it isn't fully understood. It's typically caused by an abnormal reaction to medication. Sometimes, it's difficult to identify the underlying cause of TEN.
Medication
The most common cause of TEN is an abnormal reaction to medication. It's also known as a dangerous type of drug rash, and is responsible for up to 95 percent of TEN cases.
Often, the condition forms within the first 8 weeks of taking the drug.
The following medications are most commonly associated with TEN:
anticonvulsants
oxicams (nonsteroidal anti-inflammatory drug)
sulfonamide antibiotics
allopurinol (for gout and prevention of kidney stones)
nevirapine (anti-HIV drug)
Infections
In very rare instances, a TEN-like illness is linked to an infection by a bacteria known as Mycoplasma pneumoniae, which causes a respiratory infection.
SYMPTOMS
The symptoms of TEN are different for each person. In the early stages, it usually causes flu-like symptoms. This may include:
fever
body aches
red, stinging eyes
difficulty swallowing
runny nose
coughing
sore throat
After 1 to 3 days, the skin peels with or without blistering. These symptoms can progress within several hours or days.
Other symptoms include:
red, pink, or purple patches
painful skin
large, raw areas of skin (erosions)
symptoms spreading to the eyes, mouth, and genitals
RISK FACTORS
Though anyone taking medication can develop TEN, some people have a higher risk.
Possible risk factors include:
Older age. TEN can affect people of all ages, but it's more likely to affect older adults.
Gender. Females may have a higher risk of TEN.
Weakened immune system. People with a weakened immune system are more likely to develop TEN. This may occur due to conditions like cancer or HIV.
AIDS. SJS and TEN are 1,000 times more common in people with AIDS.
Genetics. The risk is higher if you have the HLA-B*1502 allele, which is most common in people of Southeast Asian, Chinese, and Indian descent. The gene can increase your risk of TEN when you take a certain drug.
Family history. You may be more likely to develop TEN if an immediate relative has had the condition.
Past drug reactions. If you've developed TEN after taking a certain drug, you have an increased risk if you take the same medication.
*DIAGNOSIS
A doctor will use a variety of tests to diagnose your symptoms. This may include:
Physical exam. During a physical exam, a doctor will inspect your skin for peeling, tenderness, mucosal involvement, and infection.
Medical history. To understand your overall health, a doctor will ask about your medical history. They'll also want to know what drugs you take, including any new medications taken in the past two months, as well as any allergies you have.
Skin biopsy. During a skin biopsy, a sample piece of affected skin tissue is removed from your body and sent to a lab. A specialist will use a microscope to examine the tissue and look for signs of TEN.
Blood test. A blood test can help identify signs of infection or other problems with internal organs.
Cultures. A doctor can also look for an infection by ordering a blood or skin culture.
While the doctor is usually able to diagnose TEN with a physical exam alone, a skin biopsy is often performed to confirm the diagnosis.
TREATMENT
In all cases, treatment includes discontinuing the drug that caused your reaction.
Other forms of treatment depend on several factors, such as:
your age
your overall health and medical history
the severity of your condition
the affected body areas
your tolerance of certain procedures
Treatment will involve:
Hospitalization. Everyone with TEN needs to be cared for in a burn unit.
Ointments and bandages. Proper wound care will prevent further skin damage and protect the raw skin from fluid loss and infection. To protect your skin, your hospital team will use topical ointments and wound dressings.
Intravenous (IV) fluid and electrolytes. Extensive burn-like skin loss, especially in TEN, leads to fluid loss and electrolyte imbalance. You'll be given IV fluid and electrolytes to minimize the risk. Your hospital team will closely monitor your electrolytes, the status of your internal organs, and your overall fluid status.
Isolation. Since the skin damage of TEN increases the risk of infection, you will be isolated from others and potential sources of infection.
Medications used to treat TEN include:
Antibiotics. Almost everyone with TEN is given antibiotics to prevent or treat any infections.
Intravenous immunoglobulin G (IVIG). Immunoglobulins are antibodies that help your immune system. IVIG is sometimes used to control the reaction. This is an off-label use of IVIG.
TNF alpha inhibitor etanercept and immunosuppressant cyclosporine. These are promising treatments that are often recommended by experts in the treatment of TEN. This is an off-label use of both medications.
Specific body parts may need different treatments. For example, if your mouth is affected, a specific prescription mouthwash may be used in addition to other treatments.
Your hospital team will also closely monitor your eyes and genitals for signs. If they detect any signs, they'll use specific topical treatments to prevent complications, such as vision loss and scarring.
Currently, there is no standard treatment regimen for TEN. Treatment may vary depending on the hospital. For example, some hospitals may use IVIG, while others may use a combination of etanercept and cyclosporine.
Etanercept and cyclosporine aren't currently approved by the Food and Drug Administration (FDA) to treat TEN. However, they can be used off-label for this purpose. Off-label use means that your doctor can prescribe a drug for a condition that it isn't approved for if they think that you may benefit from the drug.
OUTLOOK
The mortality rate of TEN is approximately 30 percent, but can be even higher. However, many factors affect your individual outlook, including your:
age
overall health
severity of your condition, including body surface area involved
course of treatment
In general, recovery can take 3 to 6 weeks. Possible long-term effects include:
skin discoloration
scarring
dry skin and mucous membranes
hair loss
trouble urinating
impaired taste
genital abnormalities
vision changes, including loss
- 8
- 18
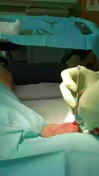
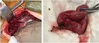
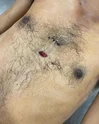
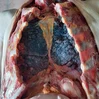
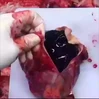
The person who murdered him took the adage “A friend in need is a friend indeed” too seriously. He was asked by the victim under the influence of alcohol to stab him superficially, so that his wife would talk to him as the deceased had a fight with his wife, and she was not talking. But his friend stabbed him much deeper piercing the sternum, pericardium and ultimately puncturing the heart at right ventricle.
The knife was also broken in the process. Then he himself took him to the hospital, where police arrested him. Images showing pierced sternum, pericardium, clot in pericardial cavity, penetration of heart and intraventricular septum, and the broken murder weapon.
- 3
- 23
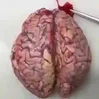
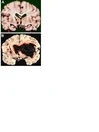
"(A) Asymptomatic intracerebral hemorrhage (arrow) localized to the left thalamus, not involving the internal capsule. (B) Massive, fatal putamenal hemorrhage with intraventricular extension, delineating the opposite end of the clinical spectrum. The satellite hemorrhage (arrow) (see text) in the fatal hemorrhage resembles the asymptomatic hemorrhage in (A)."
Figure courtesy of: Sutherland GR, Auer RN. Primary intracerebral hemorrhage. J Clin Neurosci. 2006 Jun;13(5):511-7. doi: 10.1016/j.jocn.2004.12.012. PMID: 16769513.
- 72
- 131
She had stomach pain and bloating. doctors made surgery to remove the thing blocking her track. She ate her hair for 5 years.
- 5
- 26
Kidney stones are solid deposits of minerals and salts that form in the urinary tract. These stones can cause severe pain and discomfort, and can also lead to blockages in the urinary system if left untreated.
The procedure to remove kidney stones is known as a urologic surgical procedure, and there are several methods available, including:
Shockwave Lithotripsy: A non-invasive procedure where high-energy shockwaves are used to break the stones into smaller fragments that can pass through the urinary system.
Ureteroscopy: A procedure where a thin, flexible scope is inserted into the urinary system through the urethra and bladder to visualize the stones and remove them using specialized instruments.
Percutaneous Nephrolithotomy: A procedure where a small incision is made in the back, and a scope is inserted through the incision to remove the stones.
The procedure used will depend on the size, location, and number of stones present.
Explanation of the Ureteroscopy procedure:
Anesthesia: The procedure is performed under general or spinal anesthesia, which numbs the patient from the waist down.
Insertion of the Ureteroscope: The ureteroscope is inserted into the urethra, bladder, and then into the ureter, where the stone is located.
Visualization of the Stone: The urologist uses the scope to visualize the stone and determine its location and size.
Stone Removal: Special instruments such as baskets or lasers are used to remove the stone or break it into smaller pieces that can be passed through the urinary system.
Stent Placement: After the stone is removed, a stent may be placed in the ureter to help prevent blockages and promote healing.
Recovery: After the procedure, the patient is closely monitored for any complications and may be given pain medication to manage any discomfort. Most patients can return to normal activities within a few days.
- 7
- 24
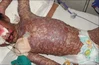
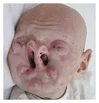
Bartsocas-Papas syndrome (BPS) is an autosomal recessive syndrome with severe craniofacial, limb, and genital abnormalities. As of 2011, 24 published cases and families were registered in the Orphanet Report Series.
Compared to other disorders characterized by pterygia, the condition is usually more severe and often lethal: most affected patients die in utero or shortly after birth. We report the first Egyptian family with Bartsocas-Papas syndrome comprising three cases; our proband who was a female infant with severe craniofacial and limb anomalies typical of Bartsocas-Papas syndrome, a similarly affected female fetus which died in utero at the 7th gestational month, and a 16-year-old mentally retarded uncle who presented with some of the typical features of Bartsocas-Papas syndrome, including syndactyly, thumb hypoplasia, and microphthalmia.
- 8
- 46
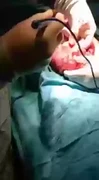
A Very large tamponade was revealed under the pericardium due to a massive amount of hemorrhage.
I would say this is most likely due to a stab wound in the chest from the (dead) victim, because of an incision in the myocardium over the left ventricle. That caused blood to move from the ventricle into the pericardium, just an observation. 






































.webp?x=8)





 Girl Dying
Girl Dying  On Drug Overdose
On Drug Overdose  (Subtitled)
(Subtitled)














 Slavshit
Slavshit

 Sandshit
Sandshit
